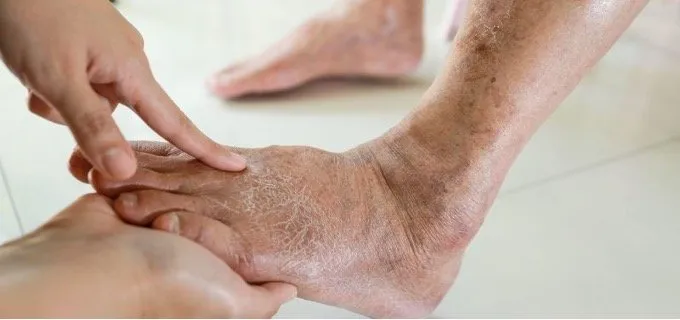
Chronic venous insufficiency (CVI) occurs when the valves in the veins of the lower legs fail to function correctly. Normally, these valves keep blood moving upward toward the heart; when they become damaged or weakened, blood pools in the lower extremities. This pooling increases pressure within the veins, which leads to physical changes in the surrounding tissues. Managing this condition requires a practical approach that supports your vascular system and adapts daily habits to meet your body’s needs. Here are some tips on how to manage chronic venous insufficiency:
Improve Blood Flow
Supporting efficient circulation is a primary focus when managing chronic venous insufficiency, and movement is a good starting management method. Physical movement acts as a natural pump for your veins. When you walk, the muscles in your calves contract and help push blood back up toward your heart. You can elevate your legs above your heart to encourage proper blood flow, and you should take regular breaks to walk if you sit for long periods. Simple ankle exercises, such as pointing and flexing your toes while seated, also engage these key muscle groups.
Improve Healing
Proper circulation directly impacts your body’s ability to heal, especially concerning the skin on your lower legs. Poor venous function can lead to skin breakdown or venous stasis ulcers, making proactive cardiovascular health invaluable. Adapting your lifestyle choices can promote circulation and improve your healing ability. Maintaining a balanced diet rich in key nutrients supports vascular integrity and promotes cellular repair. Incorporating foods high in vitamin C and zinc assists in maintaining skin health and structural protein production.
Regular exercise strengthens your cardiovascular system, but you should discuss any new physical activities with your healthcare provider first. Weight management also plays a fundamental role in healing, as maintaining a healthy weight reduces the overall mechanical burden on your lower extremity veins. Decreasing sodium intake further assists by minimizing fluid retention throughout the body.
While daily habits can impact blood flow management, professional evaluation provides regular healthcare guidance. You should visit a vascular specialist if you notice skin discoloration around your ankles, experience sudden increases in leg heaviness, or observe new varicose veins developing. A specialist can assess the specific condition of your venous valves and recommend targeted interventions to prevent further progression.
Reduce Swelling and Pain
Leg swelling, or edema, frequently accompanies CVI and contributes to general discomfort. External support methods offer straightforward ways to manage this symptom. Graduated compression stockings provide targeted pressure that decreases from the ankle upward, which helps counteract the outward pressure of pooling blood. These garments keep fluid from accumulating in the tissue spaces. Compression stockings deliver gentle pressure to lower leg fluid buildup, and they offer a practical way to manage daily discomfort.
Individuals managing venous conditions must also understand their personal risk for more severe complications, such as deep vein thrombosis (DVT). DVT involves the formation of a blood clot in a deep vein, which causes sudden swelling, acute pain, and localized warmth. Recognizing your personal risk factors, such as prolonged immobility, a history of blood clots, or specific genetic predispositions, helps you monitor your symptoms appropriately.
Manage Chronic Venous Insufficiency Effectively
To successfully treat and manage chronic venous insufficiency, you can implement various changes to your daily habits and structural support. Focusing on practical lifestyle adjustments helps support your vascular health and maintain your quality of life. A medical provider may suggest changes like prioritizing regular movement and using compression therapies, and by consistently implementing these strategies, you target symptoms while minimizing their impact on your daily routine. Contact a vascular vein specialist to learn more management strategies.