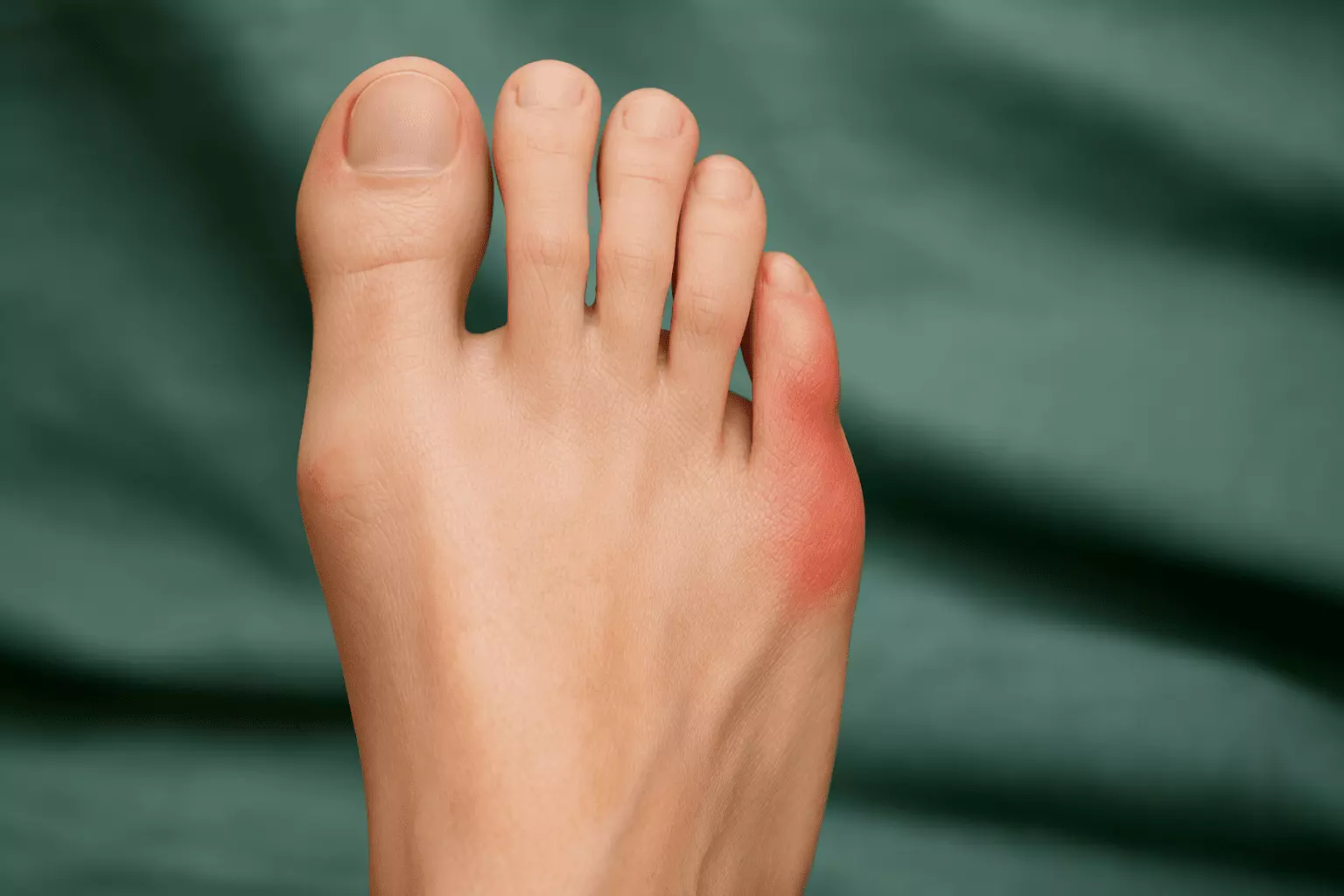
Bunions are a common structural deformity of the foot. A bony bump forms on the joint at the base of the big toe, altering the alignment of the bones. This condition develops slowly over time, and it changes the foot’s physical appearance. Understanding the anatomical changes helps patients make informed healthcare decisions.
What Are Bunions?
Bunions involve the deviation of the big toe toward the adjacent toes. The first metatarsal bone shifts outward, and the phalanx bone angles inward. This structural misalignment forces the joint to protrude, creating the characteristic bump on the inner side of the foot. The skin over the bunion may appear red, and the surrounding tissue often becomes inflamed from persistent friction.
What Causes Them?
Genetic factors play a significant role in the development of bunions, as individuals may inherit a specific foot structure prone to this deformity. Flat feet or low arches increase the risk of joint instability, which contributes to the gradual shifting of the bones. Wearing tight or narrow shoes exacerbates the underlying structural issues. Medical conditions like rheumatoid arthritis also affect joint health and can accelerate bunion formation.
What Are the Symptoms?
Patients with bunions may report localized pain at the site of the protruding joint. Swelling and redness are common signs of joint inflammation, and restricted mobility in the big toe may occur as the condition advances. Corns or calluses sometimes develop where the first and second toes rub together, adding to the overall discomfort. A visible bump on the inside of the foot is the most apparent physical sign.
How Is Daily Life Affected?
The physical symptoms of bunions impact routine activities, and patients may experience difficulty walking long distances. Finding well-fitting footwear can be challenging, as some standard shoe styles put painful pressure on the protruding joint. The resulting friction causes skin irritation, limiting participation in high-impact exercises. Patients sometimes modify their routines to minimize physical stress on the foot.
Recreational activities such as running or hiking become difficult to maintain, leading individuals to reduce their overall physical activity. This reduction in mobility can impact general cardiovascular health. The ongoing pain may lead to compensatory changes in gait. A modified walking pattern places unnatural stress on the knees and hips, and this secondary strain has the potential to lead to additional musculoskeletal problems.
What Are the Treatment Options?
Conservative management strategies aim to relieve pressure on the joint. Footwear modification is a primary non-surgical intervention that involves selecting shoes with a wide toe box. Custom orthotics provide structural support for the foot and help distribute weight evenly across the sole. Such modifications reduce the daily strain on the affected joint, so patients may report decreased localized pain.
Surgical interventions become necessary when conservative treatments fail, and these procedures aim to realign the bone structure. Arthroscopy is a minimally invasive surgical option that utilizes small incisions to correct joint deformity. Laser surgery targets specific tissues with high precision and offers an alternative approach to treating the affected area. Recovery times vary depending on the chosen procedure.
Visit a Podiatrist Today
A professional medical evaluation is the initial step toward managing this condition. Early intervention helps prevent further joint deterioration, and a customized treatment plan addresses each patient’s specific symptoms. You should schedule a consultation with a foot specialist to find appropriate therapies based on your clinical presentation. Properly managing the condition may improve overall foot health.