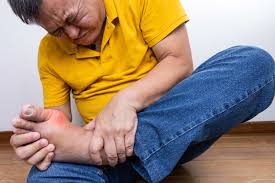
Gout is an inflammatory condition that often presents as sudden and severe joint pain, redness, and swelling. While commonly associated with certain dietary habits or advancing age, gout reflects underlying processes that affect the entire body. Its development and complications are influenced by underlying systemic conditions.
What Is Gout?
Gout is a specialized form of inflammatory arthritis that is characterized by recurrent, sudden attacks of pain, redness, and swelling. These symptoms most frequently target the joint at the base of the big toe. The physiological foundation of this condition is elevated levels of uric acid in the bloodstream. Uric acid forms when the body breaks down purines, natural substances found in tissues and many foods. When the body produces excessive uric acid or the kidneys excrete too little, the compound builds up. This excess forms sharp, needle-like urate crystals in a joint or surrounding tissue. These crystals trigger severe inflammation. Without medical intervention, episodes can become more frequent and last longer, eventually causing permanent damage to the affected joints.
What Conditions Are Related?
The relationship between gout and other medical issues is highly intertwined. Certain underlying states elevate the risk of developing uric acid crystals, while chronic inflammation associated with gout contributes to the development of other systemic problems. Chronic kidney disease stands out as a primary contributor. When the kidneys experience functional decline, they lose the ability to efficiently filter waste products, leading to a direct accumulation of uric acid in the blood. Metabolic syndromes share a deep link with this form of arthritis. This cluster of conditions includes high blood pressure and excess body fat around the waist. Medical professionals frequently observe that patients presenting with gout already exhibit signs of type 2 diabetes.
Cardiovascular disease represents a significant risk for individuals with a history of gout attacks. This vascular damage increases the risk of developing heart disease. Kidney stones represent another direct complication. Advanced gout also leads to the formation of tophi, which are visible nodules of uric acid that develop under the skin near joints. While usually painless, tophi become inflamed during attacks and can erode surrounding bone structures.
How Is It Treated?
Medical management focuses on alleviating the pain of acute flares and preventing future episodes by lowering systemic uric acid levels. To manage an active attack, physicians typically rely on medications that quickly reduce inflammation. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be utilized first. Corticosteroids offer an alternative for patients who cannot tolerate NSAIDs, providing rapid relief through oral pills or direct joint injections.
For long-term management, doctors prescribe medications designed to lower the concentration of uric acid in the blood. Certain drugs limit the body’s natural production of uric acid, while others help the kidneys remove uric acid more efficiently. Dietary modifications involve restricting the intake of purine-rich foods, such as red meat and certain types of seafood. Decreasing alcohol consumption lowers risk. Maintaining adequate hydration assists the kidneys in flushing waste products from the system.
Seek a Professional Medical Assessment
Consulting a physician delivers access to specialized diagnostic tools. These precise diagnostics confirm the presence of urate crystals and evaluate the extent of any joint erosion. Because gout signals potential vulnerabilities in cardiovascular and metabolic systems, a thorough medical evaluation guides the development of a tailored, long-term health strategy. Taking these steps helps maintain physical mobility and protects your broader systemic well-being.